
Healthcare costs rise fastest when risk is recognized late. Imaging is often where that delay begins, because scans can contain early warning signs that are not escalated quickly or followed through consistently. When interpretation slows, when follow-up slips, or when backlogs grow, clinical decisions slow down, and costs start stacking up.
Predictive analytics in healthcare reduces that exposure by identifying risk early enough for action. It uses patterns from clinical and operational data to flag which patients, findings, and workflows are most likely to lead to high-cost outcomes. The value shows up when those predictions change behavior in real time, such as prioritizing urgent reads, preventing missed follow-ups, and reducing delays that extend the length of stay.
Medical imaging AI strengthens this approach by converting imaging data into structured signals that predictive systems can use. Many healthcare teams work with partners such as Xavor to deliver Custom AI solutions that connect imaging, EHR data, and real workflows, enabling insights to drive triage, follow-up tracking, and timely escalation. This article explains how predictive analytics and medical imaging AI work together to identify risks before they become costly problems and which use cases deliver measurable impact.
What is predictive analytics in healthcare?
Predictive analytics in healthcare uses machine learning, statistical modeling, and data analysis to analyze past and current health data and estimate future outcomes. In prevention-focused care, it identifies patterns linked to future illness by assessing factors such as family history, genetics, lifestyle habits, environmental exposure, and prior medical conditions. These predictions help care teams act earlier and design preventive plans tailored to each patient’s specific risks.
If you want a broader view of the data foundation behind these predictions, explore the role of healthcare data analytics in predicting patient needs.
Why is predictive analytics important for healthcare?

Predictive analytics matters in healthcare because it supports two needs simultaneously: better clinical decisions and smoother operations. When teams can estimate health risks earlier, they can adjust care plans sooner, focus on preventive support for the right patients, and reduce avoidable hospital use, which drives costs.
Research also suggests that risk models can improve when they include social and environmental factors, rather than relying solely on clinical history. One recent study evaluated a composite socio-environmental cardiovascular risk score for forecasting major adverse cardiovascular events, showing why adding these factors can strengthen risk estimation for prevention planning.
On the operations side, predictive analytics helps plan capacity and staffing based on expected demand. In the AMN Healthcare 2023 survey, 80% of nurses expected the nursing shortage to worsen over the next five years, and a separate report on the same survey noted that about 94% of respondents reported a moderate or severe shortage in their area. Predictive models can support smarter scheduling and workload planning, so resources are used where pressure is building rather than reacting after service levels slip.
Predictive analytics is also used in public health to anticipate outbreaks and support earlier responses. For influenza, recent work has focused on forecasting hospital admissions at the state level across the season, which helps plan surges and allocate resources.
1. Effective resource allocation
Predictive analytics in healthcare helps organizations place staff, rooms, and imaging capacity where demand is likely to rise. That reduces last-minute firefighting and helps teams protect capacity during staffing gaps. One health system, Gundersen Health System, reported a 9% increase in room utilization after using AI-driven predictive analytics.
Predictive models can also flag patients who are likely to miss appointments, so schedules can be managed more intelligently, and fewer slots go unused. Over time, better allocation reduces avoidable costs and supports stronger financial performance.
2. Disease prevention and early detection
Predictive models help estimate who is likely to develop a condition based on clinical history and other relevant factors. Once a risk pattern is identified, care teams can step in earlier with prevention plans, monitoring, and follow-up. The same approach also supports early detection by highlighting subtle changes that often show before severe symptoms. Earlier action usually reduces the chance of expensive escalation later.
3. Matching patients with the right providers and treatments
When patient data is organized well, predictive analytics can support better routing. It can help match patients with clinicians who have the right expertise for a specific condition and highlight treatment options that align with the patient’s risk profile and history. This improves care planning because decisions are based on patterns in real patient outcomes, not only on general guidelines.
How early risk detection prevents cost escalation
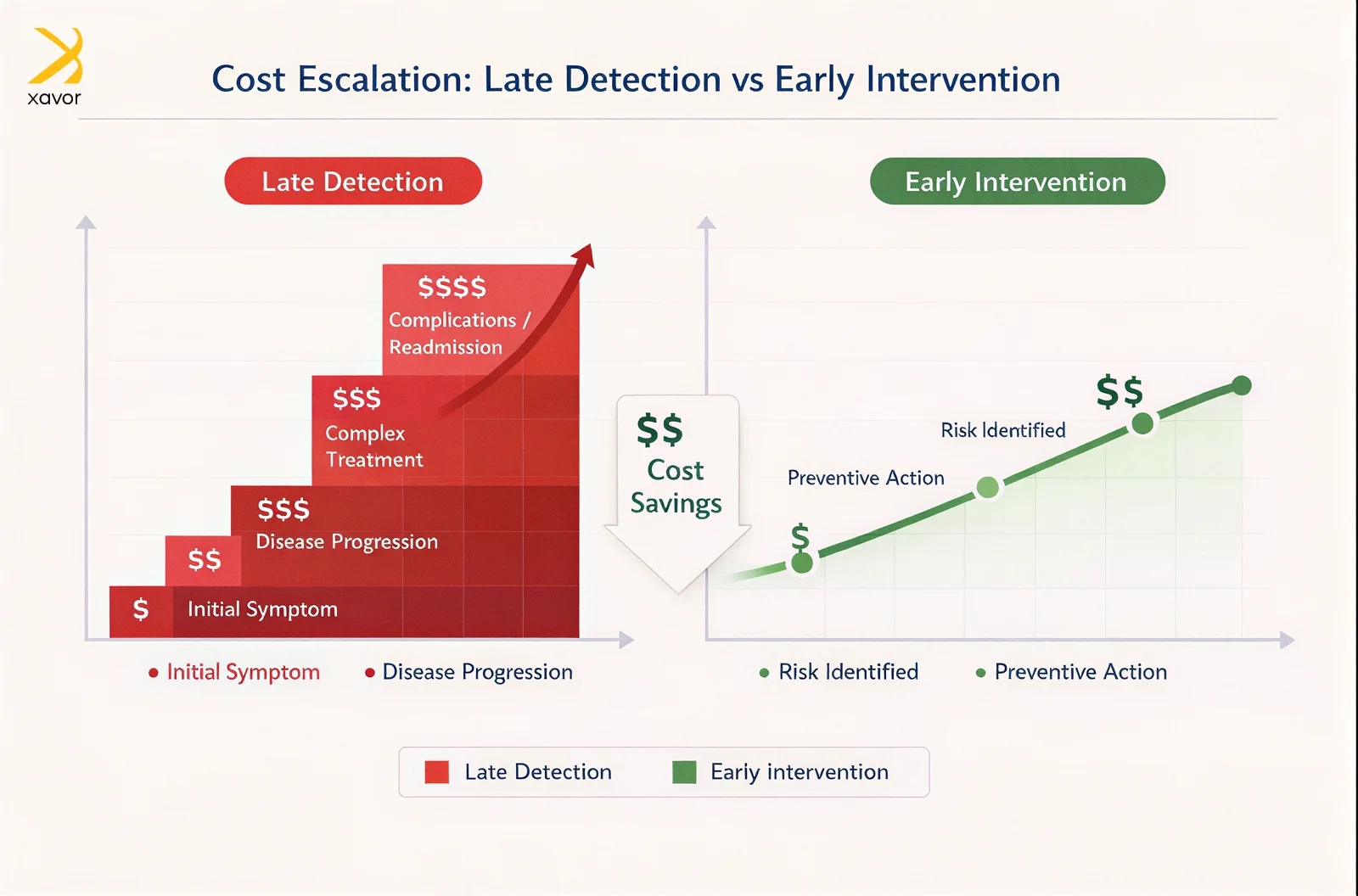
Healthcare cost pressure often comes from one problem: action is taken after the window for simple intervention has already passed. When risk is identified late, care becomes more intensive, stays longer, and outcomes become harder to control. That pattern shows both clinical risk and operational risk.
Clinical risk becomes expensive when the disease is detected after it has progressed, because treatment becomes more complex and complications become harder to avoid. Cost also rises when a patient deteriorates without timely escalation, or when discharge happens without recognizing risk, and the patient returns for readmission. Operational risk increases cost in a different way. Imaging delays can slow decision-making across the hospital, backlogs can extend length of stay, repeat MRI scans can waste scanner time, and missed follow-up recommendations can push patients into late-stage care. Emergency flow also suffers when imaging becomes a bottleneck, and boarding quickly adds cost.
Predictive analytics reduces this exposure by helping teams act while risk is still manageable. The strongest programs do not stop at risk scoring. They connect predictions to operational decision points, such as triage, escalation, scheduling, or follow-up tracking. That matters because the organization can intervene earlier, avoid unnecessary escalation, and protect capacity.
A simple test shows whether predictive analytics in healthcare is worth the investment. If the output changes a workflow that teams already run every day, it can prevent costs. Once teams use the workflow consistently, delays reduce, repeat scans drop, follow-ups get completed, stays shorten, and avoidable readmissions fall.
What predictive analytics means in day-to-day healthcare operations
Predictive analytics is often described as forecasting outcomes. In practice, it works only when prediction is linked to execution. A functioning predictive program has four components.
1. Inputs
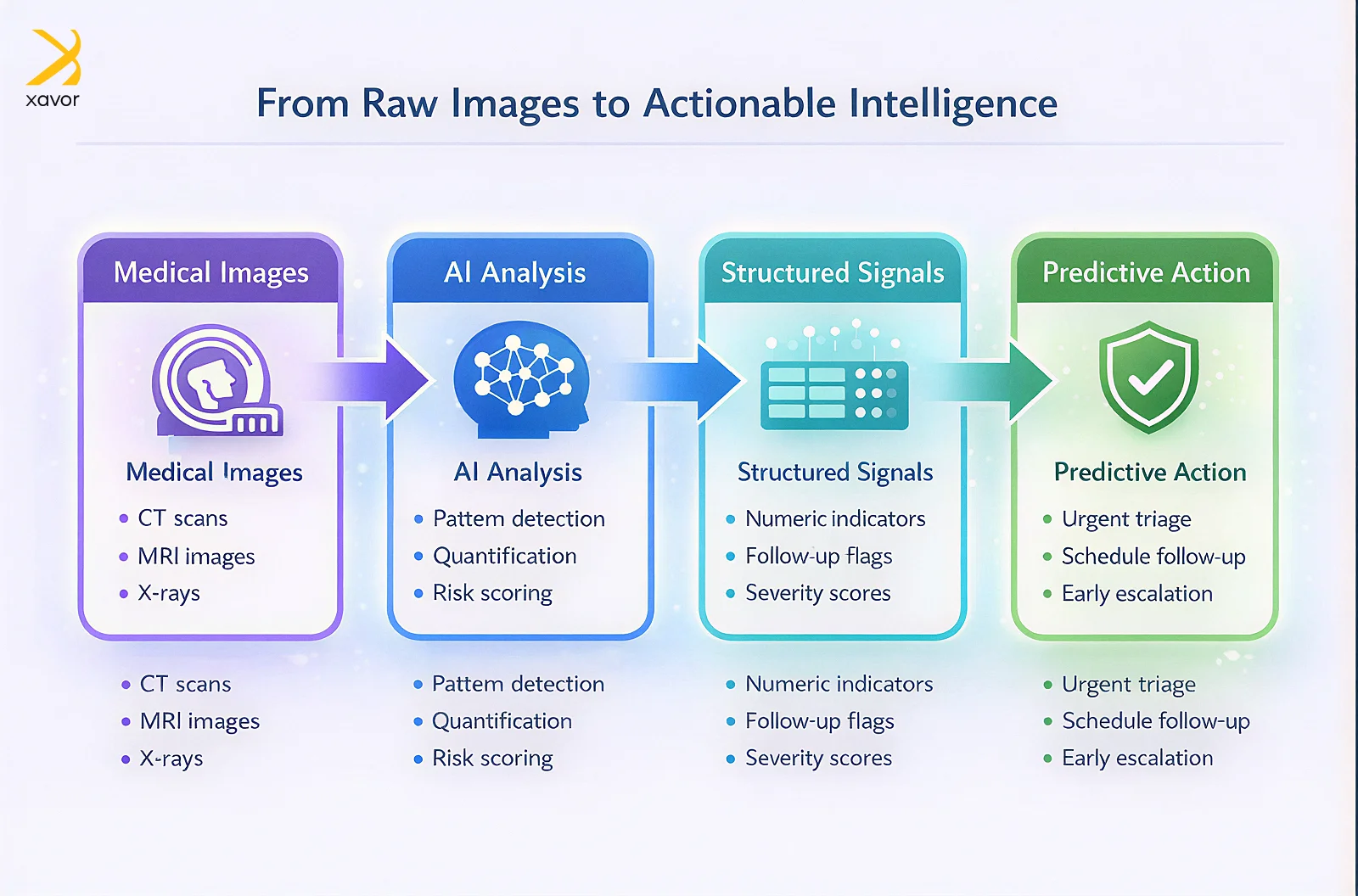
Inputs come from EHR data, labs, vitals, medications, prior utilization, scheduling patterns, and imaging. Imaging adds unique value because it provides objective visual evidence that can indicate urgency, severity, and progression.
2. Signal creation
Signal creation converts raw inputs into usable indicators. For imaging, this step is often the hardest because images are not naturally structured data. Radiology reports contain structured information only when they are written in consistent formats, and that varies widely by site and individual practice.
3. Risk scoring
Risk scoring estimates the probability of specific events. These events should be tied to cost and safety. Examples include the probability of deterioration, ICU transfer risk, probability of missed follow-up, repeat scan risk, or predicted turnaround time delays.
4. Action layers
Action layers are where value is realized. Action can include triage, escalation, scheduling, care coordination, staffing adjustments, and protocol selection. Risk scoring without action is reporting, not prevention.
Imaging-led predictive analytics has an advantage because imaging workflows already support action. Worklists can be reprioritized. Critical result protocols can be strengthened. Follow-up tracking can be automated. Operational bottlenecks can be forecasted and managed. That is why imaging is frequently the fastest path from prediction to measurable operational improvement.
Why imaging is one of the strongest early signals for costly risk
Imaging plays a unique role because it is both clinical and operational.
Clinically, imaging can show early disease detection signals before symptoms become severe. It can reveal severity and progression that determine treatment urgency. It can guide decisions in high-cost pathways such as stroke, cancer, trauma, cardiology, and infectious disease.
Operationally, imaging influences flow across the organization. Delayed reads slow emergency disposition. Backlogs extend the length of stay. Repeat imaging increases cost per study and consumes capacity. Missed imaging follow-ups increase late-stage diagnoses and unplanned utilization.
Cost often rises because of predictable failure points:
- Critical findings are present, but interpretation is delayed
- Follow-up recommendations are documented but not executed
- Imaging backlogs expand and slow decisions across service lines
- Repeat scans increase due to motion, artifacts, or protocol mismatch
- Emergency imaging delays increase boarding and extend time in the system
Predictive analytics improve when imaging signals are included, because imaging provides objective evidence that correlates with clinical deterioration and resource needs. The limitation is that imaging signals must be structured, consistent, and linked to workflows. That conversion is where medical imaging AI contributes.
What medical imaging AI adds to predictive analytics
Medical imaging AI strengthens predictive programs through practical contributions that can be measured and governed. These contributions are directly tied to time, workflow reliability, and cost prevention.
Earlier triage for time-sensitive findings
In urgent cases, time is not just a metric; it is the difference between a smooth recovery and a long, costly care journey. AI helps spot signs of serious findings early and move those scans to the top of the radiology worklist. That small shift in priority can mean a scan is read sooner; decisions are made sooner, and complications are less likely. A UK report described stroke centers using an AI tool to quickly analyze CT scans, enabling teams to begin treatment earlier. The report noted that the average time for treatment initiation dropped from 140 to 79 minutes.
Consistent quantification for longitudinal risk tracking
Predictive models improve when they use stable numeric indicators rather than variable narrative descriptions. Imaging AI supports quantification such as lesion size, growth rates, hemorrhage volume, and severity scoring. This supports risk scoring for progression and deterioration and reduces reliance on inconsistent descriptions across readers.
Report intelligence and structured extraction
Radiology reports contain many signals that drive follow-up and escalation. AI and NLP can identify follow-up recommendations, high-risk language, and structured findings, then trigger tracking workflows. This matters because missed follow-up is one of the most expensive and preventable failure points in imaging pathways.
Operational signals that predict bottlenecks
AI can support the detection of quality issues, motion artifacts, and protocol mismatches. Predictive programs can use these signals to estimate repeat scan risk, schedule drift, and backlog risk. That protects imaging capacity and reduces downstream delays that affect clinical decisions.
These contributions map directly to the benefits of AI in medical imaging that matter because they are measurable: shorter time to action, fewer preventable delays, fewer repeats, higher capacity, and tighter workflow reliability.
Use cases where predictive analytics plus medical imaging AI prevents avoidable costs
The best use cases share three traits: the risk becomes expensive when detected late, imaging provides an early signal, and the intervention pathway is clear. The goal is not to list everything. The goal is to focus on pathways where predictive workflows can prevent cost in measurable ways.
1. Stroke triage and time-sensitive brain imaging
Stroke pathways are time-critical. Imaging determines whether urgent intervention is possible and whether transfer is required. Delays increase disability risk, increase length of stay, and create long-term costs.
Medical imaging AI supports triage by identifying patterns associated with suspected hemorrhage or large vessel occlusion on CT Scan. Predictive analytics can then estimate the likelihood of deterioration and likely resource needs, which supports earlier coordination.
Action pathways that prevent cost
- Priority routing of urgent studies
- Faster escalation to stroke teams
- Earlier planning for ICU and intervention resources
- Faster treatment initiation and fewer delay-driven complications
This use case is valuable because the signal is early, the action path is clear, and the cost impact is measurable.
2. Preventing missed follow-up for incidental findings
Missed follow-up is one of the most expensive breakdowns in imaging-driven care. Incidental findings often require repeat imaging. When follow-up is missed, progression may occur silently, and treatment becomes expensive when the patient returns later with advanced disease.
Predictive analytics in healthcare helps by estimating who is likely to miss follow-up and which findings are at higher risk of progression. Medical imaging AI strengthens the approach by extracting structured finding characteristics and supporting consistent detection.
How a closed-loop workflow typically works
- AI and NLP models identify follow-up recommendations and structured findings
- A risk model estimates the probability of missed follow-up
- Outreach and scheduling are triggered for high-risk cases
- Completion is monitored, and gaps are escalated
Why is cost prevention measurable
Higher follow-up completion rates reduce late-stage detection. Earlier treatment reduces high-cost escalation. Liability exposure declines when follow-up tracking is reliable. This use case is often underestimated because it spans radiology, primary care, and care coordination, but it becomes expensive when it fails.
3. Breast screening stability and delay prevention
Screening programs depend on consistent reading capacity and timely diagnostic resolution. Delays increase risk because diagnostic follow-up slows, and detection can occur later than necessary.
Evidence from mammography screening research reported that AI-supported screen-reading procedures can reduce screen-reading workload without reducing cancer detection rate in trial settings. Reporting on the MASAI randomized trial describes increased cancer detection and reduced radiologist workload in a cohort of over 105,000 women.
Where prediction helps
- Forecasting workload peaks that cause backlog
- Identifying cohorts where delay increases risk and cost
- Prioritizing follow-up imaging and diagnostic workups
Cost prevention logic
When resolution is earlier, escalation happens earlier when needed, and expensive late-stage treatment becomes less likely.
4. MRI AI to prevent repeats, protect throughput, and reduce downstream delays
MRI is a high-cost, capacity-sensitive resource. Repeat scans waste scanner time and create backlogs. Backlogs delay diagnosis and treatment decisions, which can extend stays and increase downstream costs.
MRI AI supports motion correction, artifact reduction, accelerated reconstruction, and quality improvements. Predictive analytics strengthen the case by forecasting which patients and protocols are likely to generate motion artifacts, longer scan times, or repeats.
This is where an AI MRI reader workflow can support prioritization. When high-risk MRI studies are routed for faster interpretation, escalation decisions can occur earlier.
Practical actions that prevent cost
- Identifying motion risk early and applying corrective workflows
- Reducing repeats through quality reliability
- Improving schedule adherence through predictive control
- Prioritizing interpretation for studies linked to escalation risk
MRI-based predictive programs are often straightforward to measure because repeats, throughput, and schedule adherence are visible metrics.
5. Oncology response monitoring and progression risk prediction
Oncology becomes expensive when progression is detected late. Imaging is central to measuring response and detecting progression. Predictive analytics becomes stronger when imaging features show measurable change over time.
Medical imaging AI supports segmentation and quantification, so progression trends can be tracked more consistently. Predictive models can then estimate progression risk and support timing decisions for follow-up imaging and escalation.
Cost prevention logic
- Earlier escalation reduces unplanned admissions
- Follow-up cadence aligns with risk rather than fixed intervals
- Resource planning becomes more predictable for high-cost cohorts
This is a pathway where the signal is often present before a crisis occurs, which is where prediction adds value.
The benefits of AI in medical imaging that are measurable in predictive programs
These benefits are included because they connect directly to risk prevention and operational reliability:
- Shorter time to critical interpretation through triage
- More consistent quantification that strengthens risk scoring
- Lower MRI repeat scan rates through motion and artifact reduction
- Higher throughput and protected imaging capacity
- Lower backlog risk because urgent studies are routed earlier
Each benefit connects to cost categories: extended length of stay, boarding, repeat imaging expense, and late escalation.
How to measure impact without adding complexity
Predictive analytics powered by medical imaging AI should deliver value in the same places where delays create costs. The simplest approach is to track a few signals that show whether early imaging risk detection is turning into faster action and fewer expensive outcomes.
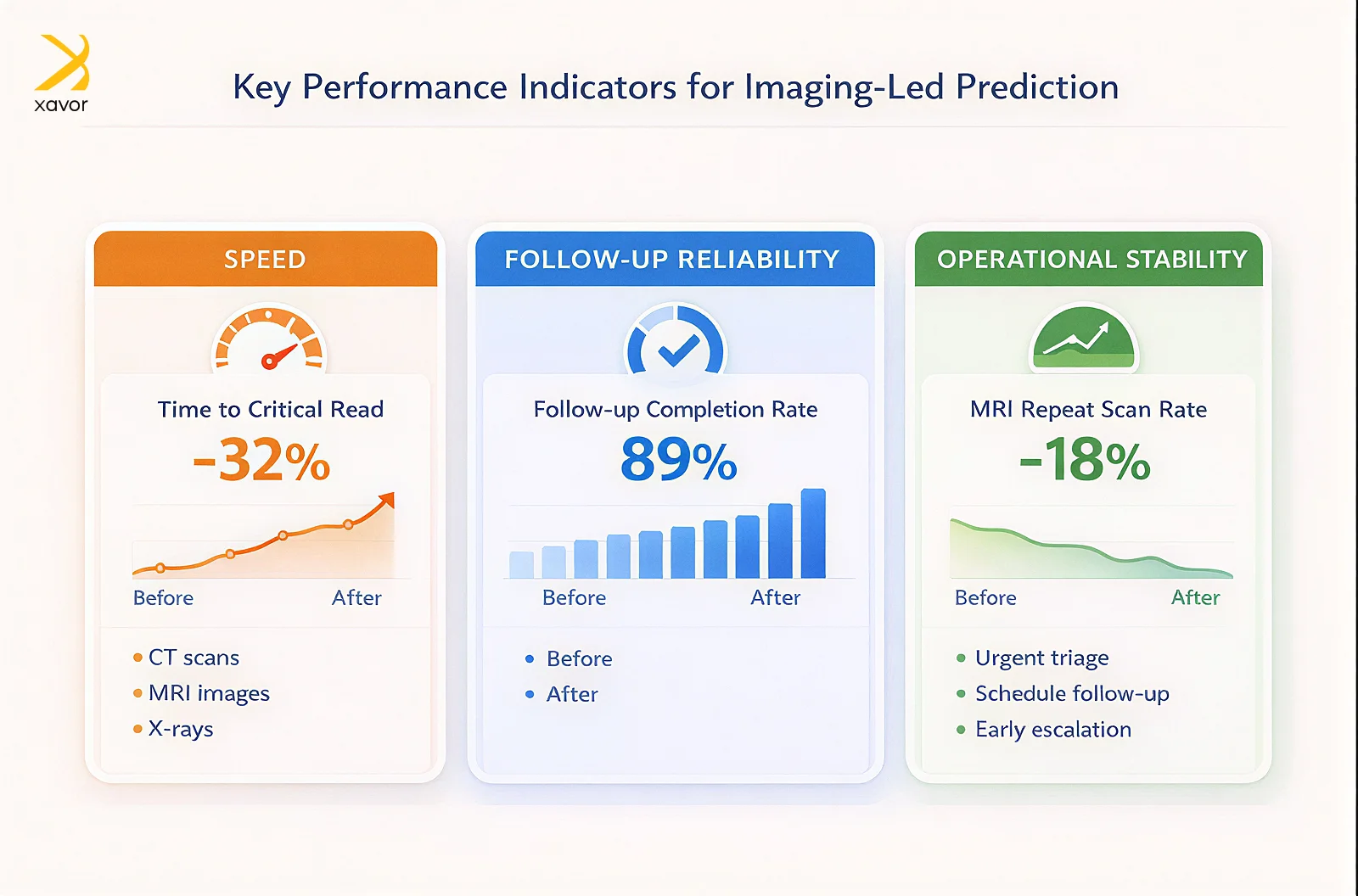
Focus on three areas:
- Speed: time from scan completion to confirmed interpretation for urgent findings, and time from imaging to treatment in time-sensitive pathways such as stroke.
- Follow-up reliability: how often recommended follow-ups are completed, and how often incidental findings fall through gaps.
- Operational stability: backlog size, turnaround time consistency, and MRI repeat scan rate when motion or artifacts drive rework.
If speed improves, follow-up gaps shrink, and operational delays reduce, then imaging-led prediction is doing what it is supposed to do. It turns early signals into earlier decisions and prevents avoidable costs.
How Xavor supports predictive analytics and medical imaging AI programs
Predictive analytics and medical imaging AI only create value when they work inside real clinical and operational workflows. Many teams face the same blockers: data sits across disconnected systems; imaging signals are not structured for prediction, and model outputs do not reach the people who need to act. These gaps lead to delayed decisions, missed follow-ups, repeat work, and higher-cost escalation.
Xavor supports healthcare organizations through Custom AI solutions that connect imaging, EHR data, and real workflows so predictive insights can drive triage, follow-up tracking, and escalation on time. The delivery focus stays practical by tying implementation to measurable outcomes, such as turnaround time, follow-up completion, backlog stability, repeat scan reduction, and length-of-stay impact.
Conclusion
Cost pressure often begins when early warning signs fail to prompt early action. Imaging is a common point where that gap appears because findings can be urgent, but interpretation, escalation, or follow-up can still move slowly. When those steps lag, patients progress into higher-cost care, and the system absorbs avoidable delay.
Predictive analytics reduces that exposure by estimating which imaging findings and workflow points are most likely to escalate into costly outcomes. Medical imaging AI strengthens this by turning scans and reports into structured signals that can be prioritized, tracked, and routed to the right teams. When that connection is built into daily workflow, risk is addressed earlier, and cost prevention becomes measurable.
If you want to apply this approach, start with a small set of imaging-driven use cases where timing clearly affects cost, then connect prediction to defined actions such as urgent triage and closed-loop follow-up. Keep measurement simple, so progress is easy to validate and scale across sites. For support with planning and implementation, contact [email protected].
FAQs
AI is used to detect and quantify findings in scans, prioritize urgent studies in radiology worklists, and extract follow-up recommendations from imaging reports. These signals can feed predictive analytics, so teams act earlier on high-risk cases, reduce delays, and prevent missed follow-ups that later drive higher-cost care.
Predictive analytics can flag patients likely to deteriorate, imaging studies likely to contain urgent findings, cases at risk of delayed interpretation, and patients likely to miss follow-up imaging. It can also forecast operational risks such as backlog growth, turnaround time delays, and MRI repeat-scan probability.
Track whether early imaging signals lead to earlier action and fewer expensive outcomes. In practice, that means monitoring time to confirmed interpretation for urgent studies, follow-up completion for recommended imaging, backlog and turnaround time stability, MRI repeat-scan rate, and the impact of length of stay on targeted cohorts.

