
Electronic health records (EHRs) have carried the baton of patients’ health records for well over decades. But it’s time to pass the baton as in the next decade or so, most medical information will be stored on the cloud or on a patient’s mobile.
And that shift is already underway as cloud computing in healthcare is becoming ubiquitous. According to a 2023 PwC report, 81% of healthcare leaders have adopted cloud computing in some aspects of their business. However, this change also requires a shift in mindset of how we approach healthcare.
Managed cloud service providers will explain to you all the benefits of cloud computing in healthcare. And all of that is important, but you should know each and everything about healthcare cloud usage before you join the other side.
That is why in this blog, we will discuss the details about cloud computing in healthcare, what it is, benefits, challenges, and future trends.
What is cloud computing in healthcare?
Hospitals typically like to keep their information in-house on personal computers. Naturally, because healthcare data is sensitive and they don’t want any outsider poking around with their patient data. But due to the gargantuan amounts of data in healthcare, they are now driven to store their information on cloud storage options.
That means moving a bunch of things, like:
- EHRs
- Imaging
- Scheduling
- Medical billing
- Telehealth analytics
There are three main cloud models that healthcare organizations opt for: public, private, and hybrid cloud. Public cloud platforms include providers like Azure, AWS, and Google Cloud. Most clinics and hospitals rely on these public cloud platforms; however, private cloud is the better option for regulated environments.
Why is healthcare moving towards the cloud?
Data is at the heart of this change. The old way of managing healthcare data is expensive and slow. Everyone is sharing more information now, and “30% of all world data is generated by the healthcare industry.” Storing and sharing this sea of information on internal devices is creating an unnecessarily complex system.

Moreover, healthcare is now focusing on predictive care. But catching diseases early on requires data processing, a lot. Cloud computing in healthcare gives computing power and flexibility to meet these demands smoothly and efficiently without the banes of in-house data storage.
Major benefits of cloud computing in healthcare
Cloud computing in healthcare can bring some wonderful results. The benefits of cloud computing in healthcare are great value for money. The upfront investment isn’t that much compared to other options, and you can see a visible difference within months.
1. Better data storage and access
Back in the days, patient information was stored in towers of paperwork. Then came onsite servers that improved things a lot. But with time, onsite storage options too started to show inefficiencies under increased workloads. Furthermore, onsite servers are pretty prone to cybersecurity threats. And no industry can afford data breaches, especially healthcare.
Cloud computing in healthcare gives you much more scalable, flexible, and secure storage options. It’s not error-free since cloud models aren’t immune to security threats or performance issues. That’s why we have cloud security in healthcare. But they are certainly a practical improvement over systems that were never designed to carry the weight we now place on them.
To give you one of the common examples of cloud computing in healthcare, a hospital may want to pull up patient records remotely, so the multiple providers in its organization can coordinate. For this purpose, they can implement any cloud model, public or private, and integrate the cloud resources in such a way that the same current information is accessible when needed.
2. Lower operational costs
A great deal of spendings on IT infrastructure in healthcare organizations is avoidable. This isn’t 2006 anymore where you need to purchase and install more pieces of hardware every time demand grows.
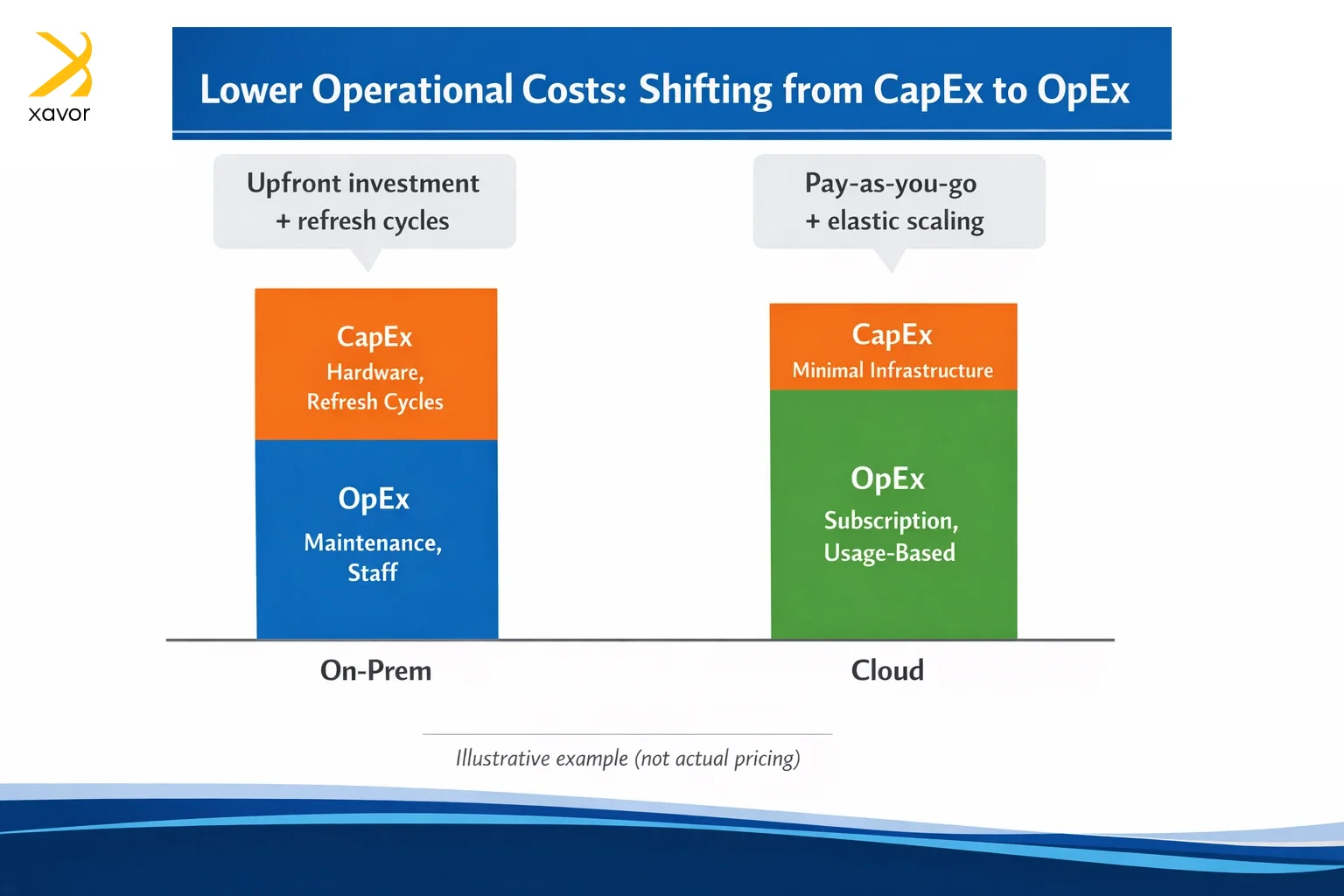
Legacy systems are costly not only because the hardware ages, but because they demand constant attention, such as:
- Maintenance contracts
- Licensing renewals
- Security patching and upgrades
Healthcare providers signed up to run hospitals, not data centers. That is why using cloud computing in healthcare is a much better financial model. Managed cloud services usually offer a subscription-based or pay-as-you-go model. Therefore, you don’t have to pay for large upfront investments. You pay for the computing and storage you actually use that can be scaled up or down without purchasing new hardware first. In practical terms, this improves cost control because spending becomes more predictable, and waste becomes easier to identify and reduce.
The savings show up in two forms. First, direct savings. The organization reduces or avoids:
- Major hardware purchases and refresh cycles
- Onsite storage expansion projects
- Maintenance and licensing costs tied to aging infrastructure
- The need for large internal teams dedicated to keeping physical systems running
Second, opportunity savings. Cloud platforms can shorten timelines for launching new healthcare services, expanding into new locations, or supporting new care models. That speed matters.
Cloud computing in healthcare is mostly about arithmetic and friction removal. But in healthcare, removing friction is sometimes the closest thing we get to progress.
3. Improved patient care
Right now, patients in the US are not exactly happy with the healthcare system. According to the State of the States 2025 survey, “Americans gave the nation a C for the overall healthcare system.” So, it is safe to say that there is a massive room for improvement.
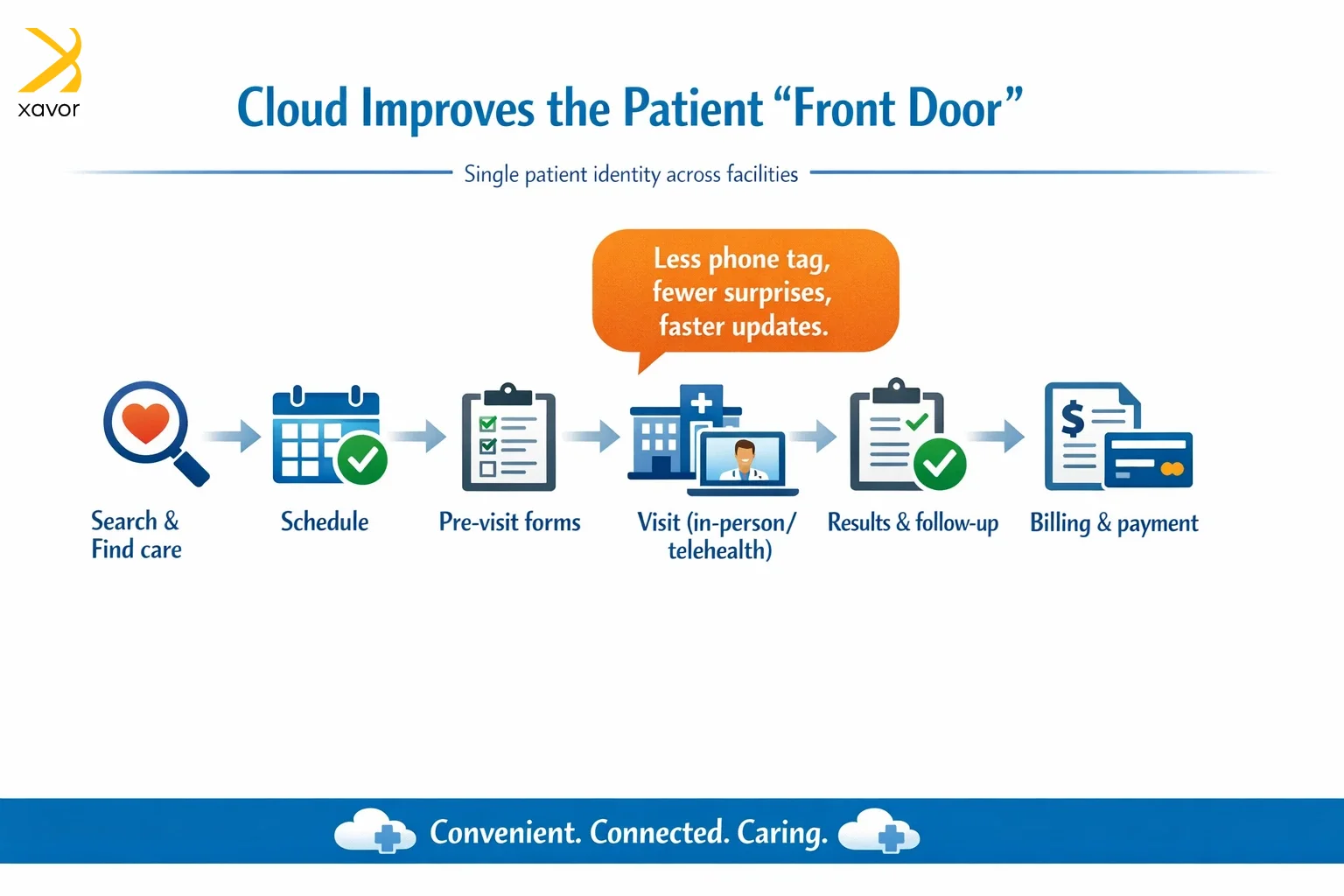
When healthcare organizations use the cloud with a patient-first approach, they can deliver the practical things patients have come to expect in every other part of life:
- Personalized health dashboards that show what’s important without making providers and patients look for needles in a haystack.
- Online portals that give access to historical records, scheduling, and updates that do not require three phone calls a day.
- Healthcare providers are also adopting secure SMS communication to improve appointment reminders, patient follow-ups, and care coordination, with platforms enabling healthcare text messaging helping organizations deliver timely updates while maintaining compliance and improving patient engagement.
- Medical billing and payments that are clear and navigable, so patients know what they owe and why.
Cloud computing in healthcare can also promote more patient engagement because when they can track everything, they are more likely to engage and follow care plans correctly.
On the provider side of things, the cloud also gives hospitals and clinics access to heavier solutions, such as data analytics, AI, and predictive models. AI-powered clinical decision support systems (CDSS) are interlinked with cloud infrastructure management to help clinicians make safer, faster decisions, especially when time is short, and the patient is complicated. Furthermore, cloud-based EMRs are much better than their onsite counterparts. They give hospitals the agility and scalability to handle workloads across locations and the ability to increase their AI adoption rate.
Major challenges in the way of cloud computing in healthcare
The grass is definitely greener on the cloud side, but the benefits of cloud computing in healthcare shouldn’t make you oblivious about its challenges and risks. Real-world implementation of cloud technologies is tricky, technical, and time-taking.
Data privacy and security
Healthcare data is the kind of information that can ruin lives when mishandled. And cloud makes it remarkably portable, which makes it attractive to criminals to exploit an expose. In 2023, the data breach at the American biotechnology company, 23andMe, leaked the profile and DNA information of millions of users on the black market. Court investigations found that the company didn’t have adequate data protection and ignored warning signs.
23andMe and many other genealogy companies beefed up their security after this attack, but the damage is done. People already trusted these companies with trepidation, and this episode only added to their fears.
AWS, Azure, or whoever is your cloud provider, they only handle the “provider side” of security: physical data center security, core encryption capabilities, and the sorts. Rest is on healthcare organizations to secure what it builds in the cloud.
You can address security challenges in healthcare cloud computing with:
- Identity and access management (IAM)
- Encryption and two-factor authentication
- Monitoring and threat detection
- Audit logging and compliance monitoring
Regulatory compliance
Compliance in healthcare is non-negotiable. Any technology that you use in your healthcare workflows must work within the boundaries set by regulatory bodies. In the US, HIPAA is the baseline requirement for protecting patient health information (PHI), and non-compliance can lead to penalties and loss of trust.
Cloud providers support HIPAA-aligned usage and offer documentation about what services are in scope, but the organization still has to design and configure the workload correctly.
The most critical responsibility on your part is cloud governance. You need to define clear ownership of who is responsible for what, plus continuous verification that the environment still matches policy after hundreds of changes.
Migration and legacy system integration
It is normal for even a small clinic to have dozens of systems to run their daily operations. And healthcare has a love-hate relationship with adopting new technologies. There are plenty of legacy on-premises platforms still used, which are not built for cloud-native integration.

Therefore, be ready to integrate or migrate disparate systems when you implement cloud computing in healthcare. The most optimal way of handling this challenge is in phases. Whether you’re migrating or integrating using the cloud, target important services first; others can remain on-prem until they are re-architected.
If it is too expensive or time-consuming for your internal team, partnering with integration services is the smarter choice.
Operational change and skill gap
That love-hate relationship healthcare has with new technologies is partially because of the institutional inertia in the industry. Doctors, nurses, and paramedical staff are very skeptic about adopting new methods in their workflows. They are comfortable with and trust their time-tested approaches.
But cloud computing in healthcare introduces new concepts and new methods. And a healthcare team is excellent at on-prem IT is not automatically equipped for cloud architecture.
This can gap can raise its head while planning and execution of ongoing operations within the cloud environment. This is why many healthcare organizations work with staff augmentation services to fill skill gaps, or to train internal teams, so ownership can eventually return in-house.
What will cloud computing in healthcare look like in five years?
What’s the road ahead for cloud computing in healthcare? The next five years for cloud computing in healthcare will be about these five things.
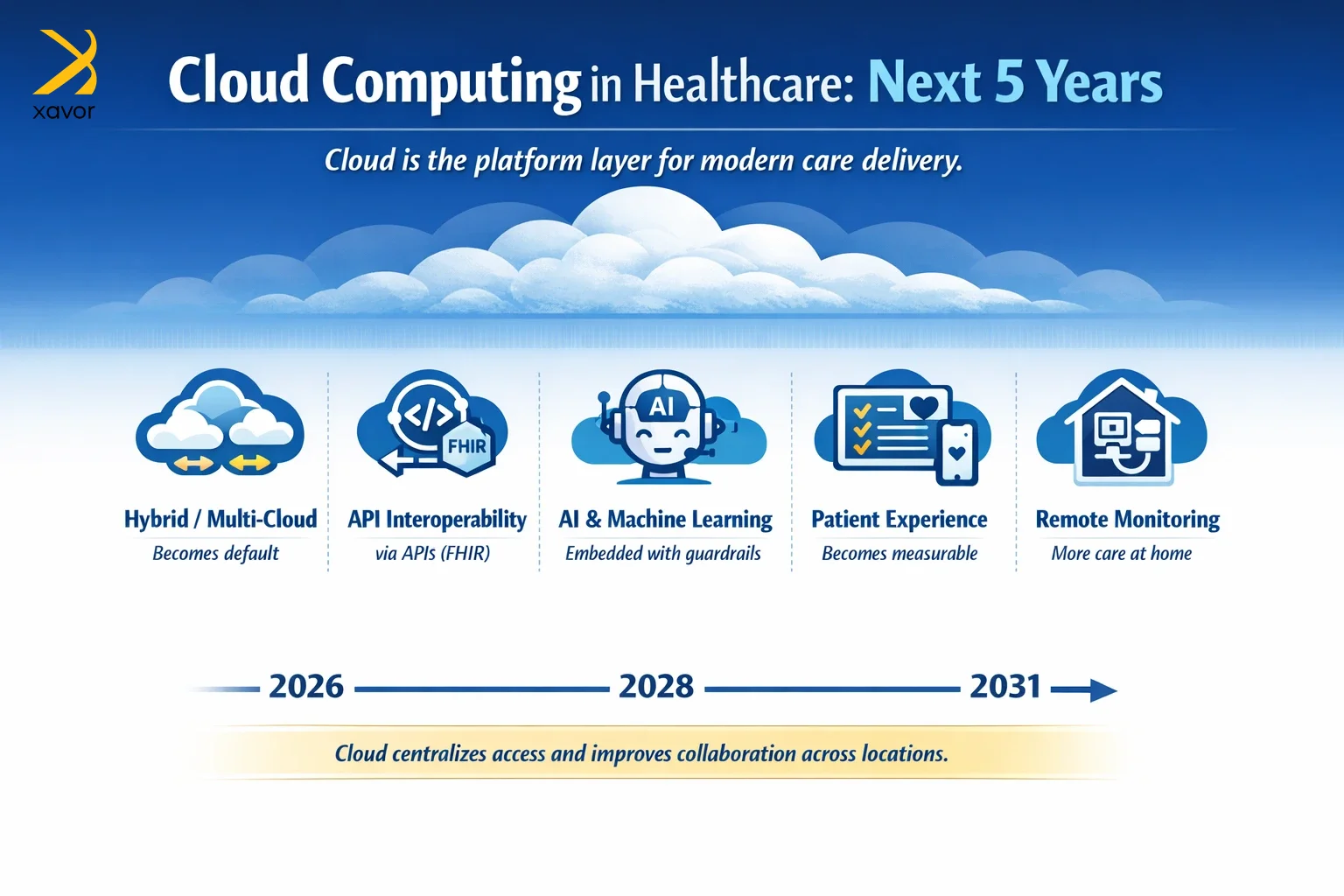
1. It becomes a matter of when, not if
Most organizations won’t be asking whether to use the cloud. They’ll be deciding which parts must remain local, and which parts belong in managed services because nobody wants to run their own mini–data center anymore. In our opinion, the common end state will be hybrid or multi-cloud models.
2. Interoperability will be the norm
A large driver will be policy pressure and market expectation around FHIR-based exchange in healthcare cloud computing. In the U.S., the CMS Interoperability and Prior Authorization Final Rule (CMS-0057-F) is already pushing the industry toward more standardized, API-based exchange and electronic prior authorization. CMS announced the rule in January 2024. Deadlines begin in 2026, and some API requirements extend beyond that, which means the next five years will be full of cloud-backed integration work.
3. Cloud will revolve AI and machine learning
Healthcare will keep adopting AI for triage, documentation support, risk prediction, and a plethora of other workflows.
The ONC HTI-1 Final Rule explicitly advances algorithm transparency and updates the certification program and information sharing expectations. In parallel, the NIST AI Risk Management Framework (AI RMF) has become a reference point for thinking about AI risks in high-stakes settings.
All of that means that cloud computing in healthcare will increasingly need guardrails as standard requirements.
4. Patient experience will be the gold standard
Portals, scheduling, messaging, and medical RCM solutions will increasingly operate on cloud-native stacks because patients expect consumer-grade convenience and because value-based care makes experience measurable. The better systems will use cloud to unify the patient’s “front door” across facilities, so the patient doesn’t feel like they’re visiting a different country every time they visit a different clinic.
5. More care happens outside hospitals
The proliferation of remote monitoring, telehealth models, and distributed care teams will keep growing, which means healthcare data will be generated at the edge and coordinated in the cloud. Therefore, expect cloud computing in healthcare to become more resilient and monitored.
Conclusion
Healthcare is changing its relationship with information. For decades, data has been treated as a byproduct of care. But with cloud computing in healthcare, it is now an active asset. It needs to be continuously available, continuously analyzed, and is increasingly essential to how care is delivered
Now keep this in mind that cloud transformation is not a one-time thing. It is a long-term capability that needs a strong architecture, thoughtful security, careful integration, and change management that respects clinical realities.
Xavor’s managed cloud services can help you build a healthcare-grade cloud foundation like that on public, hybrid, or private platforms. We have worked with Fortune 500 healthcare companies handle their cloud infrastructure, so they can focus on care.
Drop us a line at [email protected] to a book a free consultation session.
FAQs
Cloud computing in healthcare offers benefits like scalability, remote access to patient data, faster collaboration, lower infrastructure costs, and improved support for telehealth and analytics. But it also comes with challenges such as data privacy and compliance risks, potential downtime, vendor lock-in, and the need for strong security controls.
The four main types of cloud computing are public cloud, private cloud, hybrid cloud, and multi-cloud. Public cloud uses shared infrastructure from providers like AWS, Azure, or Google Cloud, private cloud is dedicated to one organization, hybrid cloud combines on-prem and cloud environments, and multi-cloud uses services from multiple cloud providers.
Recent market reports estimate the global healthcare cloud computing market at roughly $45B–$55B in 2025, with forecasts commonly projecting it to reach about $90B–$200B+ by 2030–2032 depending on how each report defines the market.

